Returning to Nyankunde
“I think that there is not a single place on earth that Jesus wouldn’t go to reach somebody.”
Christian Health Service Corps surgeon Dr. Warren Cooper and pediatrician Dr. Lindsey Cooper could have abandoned their work as medical missionaries in the Democratic Republic of Congo – one of the world’s most dangerous countries – long ago.
In fact, they’ve had plenty of legitimate reasons to leave their post at Nyankunde Hospital in the northeastern corner of the DRC since first arriving in 2013. Tribal conflicts echoing from wars beginning in the late 90s persist throughout the country, especially in the DRC’s eastern regions, which caused the destruction of the hospital in 2002 and forced the Coopers to return to the US indefinitely in 2021.
But saying goodbye to Nyankunde for good wouldn’t have sat well with the couple and their son Emmanuel, even as other medical missionaries decided to not return. Around one year after local violence forced them out, the Coopers came back to the DRC this past March, immediately resuming their work performing life-saving surgeries and educating local families on nutrition.
“It’s a tough place to serve, but it’s a place that’s become our home,” Warren said. “Even with the challenges, we feel invested, we feel like we’re part of the community. If we were to just pick up and leave and go somewhere easier, we would feel like we were missing something that was very much part of who we are, and who we have become.”
Warren and Lindsey hit the ground running with hospital work immediately upon their return. As soon as Warren first entered the building during a short visit in February, he recognized “the smell of rotting flesh” coming from a man suffering from flesh-eating bacteria, the surgeon recounted in a blog entry earlier this year.
Like so many other young men in the region, this man had been involved in tribal militias that incorporate violent beatings for punishment and ritual healing practices which can do more harm than good. He had multiple cuts on his leg where a traditional healer attempted to remedy swelling. Warren had to amputate the leg at the hip, then remove more dead tissue, but he died a few days later.
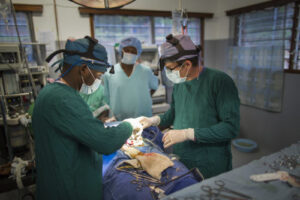 The Coopers routinely confront the physical effects of tribal violence in the form of gunshot wounds and injuries, though the conflicts take a spiritual toll as well. Warren and Lindsey say they’ve noticed a resurgence in traditional religious practices like ancestor worship and superstitions about bodily health among those involved with fighting, which is felt even by those in the local Christian church.
The Coopers routinely confront the physical effects of tribal violence in the form of gunshot wounds and injuries, though the conflicts take a spiritual toll as well. Warren and Lindsey say they’ve noticed a resurgence in traditional religious practices like ancestor worship and superstitions about bodily health among those involved with fighting, which is felt even by those in the local Christian church.
Some of those superstitions can exacerbate local health problems, Lindsey said, like a belief that malnourished babies or those with chronic conditions are cursed and cannot be touched.
“It’s a self fulfilling prophecy,” Lindsey said. “You don’t touch the child who’s malnourished, or who has wounds and needs care and of course they’ll die.”
Rather than shy away from directly addressing local conflicts, Warren and Lindsey aren’t afraid to speak out against the forces driving up hospital visits and marring the overall health of their community. They feel respected enough among the local people and leaders to contribute their perspective on touchy subjects, or to question patients involved with rebel groups about their faith.
“Is it a risk to be in a community that has armed groups? I suppose it is. But we have a voice because we’re here. And if we’re not here, we don’t have a voice into it,” Lindsey said. “When you leave a situation, it’s easy to say, ‘Oh, I’m done with that.’ But I don’t think Jesus ever really did that. The Pharisees and the Sadducees were totally lost causes, but he remained in relationships with them until the very end. And he found unexpected reception from some of the most rebellious in society. I think that there is not a single place on earth that Jesus wouldn’t go to reach somebody.”
Hunger
War isn’t the only problem the Coopers face at Nyankunde, but it touches everything, like food security. The surrounding region, like much of sub-Saharan Africa, faces issues of malnutrition due to a multitude of factors.
In the eastern DRC specifically, malnutrition is exacerbated by fighting, frequent pregnancies, and the separation of families, when fathers who do much of the farming of staple crops leave their homes to work in more profitable jobs like gold mining. As a result, many mothers are left caring for children without the ability to work the fields.
Lindsey sees the end result of food insecurity issues when working with Nyankunde’s Labor of Love program, which provides emergency feeding for people with severe cases of malnutrition, and nutritional planning for their families so they can prevent malnutrition at the home.
The program mostly serves children under the age of five, but in the case of Shekina, severe malnutrition can persist for years, with dire consequences.
Lindsey met Shekina when she was hospitalized for malnutrition at five years old. Shekina lives with often uncontrolled diabetes due to her family’s lack of access to insulin, as well as an inability to properly store insulin whenever they do have it.
Her body can’t sufficiently absorb calories without insulin, and although Nyankunde keeps plenty in stock, her family lives 10 kilometers away from the hospital.
“She had no fat in her cheeks. She had no muscle tone in her face – nothing,” Lindsey said. “You could see even her glands. She was like a walking skeleton. She didn’t really have the strength to sit. Her mom would take her in this little chair onto our indoor Children’s Garden playground area. She watched the kids play, but she had no energy to do anything.”
Shekina would receive therapeutic re-feeding at Nyankunde, but only for so long. She would have to return home after several weeks, back into a situation that continually deprived her of lifesaving medication and proper nutrition. She would be hospitalized in Nyankunde two more times, with the last visit occurring this past March.
When Shekina last saw Lindsey, she weighed 8 kilos at eight years old – as much as a healthy newborn.
“She was with us for two months. She gained almost half of her body weight again and began controlling her diabetes to the point where she could go back home,” Lindsey said.
Despite the success of Nyankunde’s efforts, the hospital cannot fully address the structural disparities that prevent kids like Shekina from accessing insulin or healthy food. In addition to being far away from a place to buy the medication, her family lacks a refrigerator to store insulin, opting instead to keep it in a clay pot of water.
Lindsey and her colleagues can counsel families on strategies to keep their children fed, whether that means addressing what foods they can find, prepare and serve, or how to best to keep diabetes under control through meal timing or avoiding sugary starches.
This counseling ensures families at least have more information on how to prevent or cope with malnutrition, which can save lives even while kids like Shekina can’t make it to the hospital.
 Warren, Lindsey and Emmanuel do see hardships as a medical missionary family, and as they’ll tell you themselves, the job can be stressful – especially when trying to solve problems without the resources doctors in developed countries are accustomed to. Even so, the beauty, serenity and positive experiences they’ve encountered working in the DRC outshine their hardships, and God has kept them safe thus far.
Warren, Lindsey and Emmanuel do see hardships as a medical missionary family, and as they’ll tell you themselves, the job can be stressful – especially when trying to solve problems without the resources doctors in developed countries are accustomed to. Even so, the beauty, serenity and positive experiences they’ve encountered working in the DRC outshine their hardships, and God has kept them safe thus far.
Returning to Nyankunde, as much as it may seem like a hassle, almost feels like a sigh of relief for the Coopers.
“People make it sound like mission work is all sacrifice and suffering,” Warren said. “But I feel like we actually have a very enjoyable life here. We live in a beautiful place. We have good friends. We have ties to the community. We have a family here. We’re involved with teaching our son and seeing him growing up and having these wonderful experiences.
“I really feel at the end of the day, that God is using us for a purpose, and it’s fun, you know?”






