Everyone around the world needs access to reliable emergency medical care, but far too many people live in places with no capacity for emergency medicine. Over 25 million people die each year, mostly in low- and middle-income countries, because they cannot reach reliable emergency medicine. These deaths represent over half of the world’s yearly mortality rate.
Emergency medicine is one of the highest priorities for healthcare development in our partner hospitals. CHSC General Surgeon Dr. Beth Stuebing knows this firsthand, given her experience in the intensive care unit of Nkhoma Hospital, Malawi.
In March, a woman arrived at Nkhoma Hospital with severe bleeding in her esophagus, likely due to untreated infections from parasites. An endoscopist attempted to locate the source of the bleeding, but it was so severe that he referred her to intensive care. He found she had an extremely low hemoglobin of 3.5.
“She was probably going to die on the table,” Beth said.
Beth took over her case in the newly constructed Nkhoma ICU, where the woman received two liters of blood transfusions and gradually became stable.
After the other hospital staff dispersed around lunchtime, Beth and another colleague stayed behind with the woman. Their rest didn’t last long. Soon she was vomiting blood again, losing around half of her blood volume.
Beth quickly called for hospital staff to return from lunch and head to the theater. She received more examinations of her esophagus (EGD), and hospital staff placed special rubber bands on the bleeding areas and injected a sclerosing agent to shrink her abnormal blood vessels.
The endoscopies showed the woman had esophagal varices–signs of portal hypertension, or scarring and fibrosis of her liver.
“That [was] from untreated schistosomiasis, which is very, very common in the rivers and Lake Malawi,” Beth said. “People get schistosomiasis as children and it’s never treated. Then they end up in liver failure with these very dangerous varices at the age of 20 or so.”
Once again, the team worked to stop the woman’s bleeding with more esophageal banding and sclerosing agent injections. Fortunately, Nkhoma Hospital had some stock of bands, fresh blood and capable physicians to quickly get the woman into a stable condition.
She ended up receiving a total of eight units of blood–more than her entire blood volume–but still ended up with a hemoglobin level of around 6, or about half the normal level.
“The ability to do this emergency endoscopy on an intubated patient who’s actively bleeding and put bands and inject the sclerosing agent is, to my knowledge, the first time that something like that has happened in Malawi, especially on somebody so sick and about to die,” Beth said. “Despite our many struggles, it’s teamwork like this that keeps us going. We had four surgeons, three residents, over three ICU nurses, two anesthetists, and several other theater staff all working for one patient.”
Even though the team was using sclerosing injections as a “last ditch effort,” Beth said, the woman survived and left the hospital several days later. Beth said this was the first time she witnessed such a dramatic case of blood loss end up in survival.
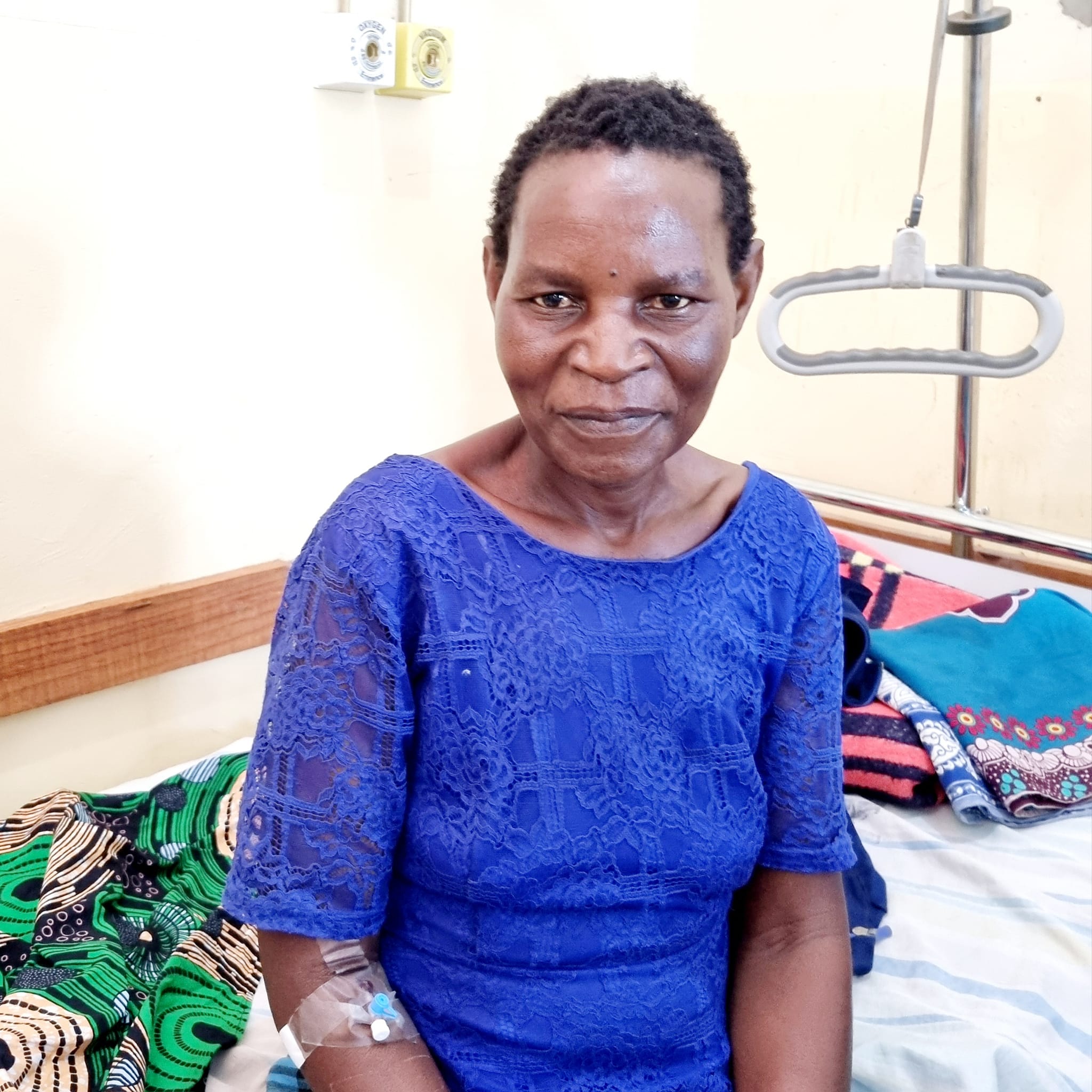
The woman underwent emergency surgery on a Friday. When Beth saw her again the next Monday, she was looking “sparky.”
“She had this cute, sheepish smile, like, ‘Yeah, I know, I’m not supposed to be here, but here I am,’” Beth said. “We were all just rejoicing. It was still unbelievable what she had come through. I think it was really a good win for the whole ICU staff, the whole theater staff. We have had a lot of [un]happy endings recently… seeing something like that happen in the Malawian context was really important for everybody to see.”